Joining forces for health care
Eight million inhabitants living in ten border regions across four countries: this is the area supported by the Hungary-Slovakia-Romania-Ukraine (HSRU) ENI CBC Programme, a largely rural environment, where a decreasing, aging population is troubled by a higher unemployment rate and a lower economic performance compared to the national averages. In border regions, people health status is in general less favourable than in central ones, particularly for the most impoverished categories. Socioeconomically precarious citizens are always the most vulnerable, but a big segment of the population at large does not lead a health-conscious lifestyle, neither seems aware of the role of prevention. All the more reason to invest in the development of health infrastructure, services, trainings programmes, prevention activities, general public awareness. That is why – when the 2014-2020 programming cycle started – the territorial cooperation between European countries and their neighbours decided to put the health care of inhabitants from the border regions among its priorities. It was crucial to devote cooperation efforts to improve the availability and level of health services and preventive activities, and since 2014 “we have supported the implementation of health projects with 12,3 million € – says Nikoletta Horvàth, deputy head of the programme’s Managing Authority – which represent close to 20% of the total available funds”.
A general upgrading of capabilities and potential
Today the ENI CBC programming cycle has started its winding down activities, and it’s time to take stock of accomplishments, and to reflect on achievements and lessons learnt during the life of the programme. In the last eight years – thanks to the financial support and the exchange of experience among partners – health stakeholders have embarked on a reciprocal upgrading of capabilities and potential. And never a time was more complex for attaining such a goal. In January 2022, the COVID pandemic had barely subsided when the Russian aggression on Ukraine was let loose, burdening the health sector throughout the country with an ongoing conflict. This sequence of crises has multiplied the urgency and needs, let alone the strains on the system.
 Within the frame of the HSRU ENI CBC Programme, hospitals from the four countries have formed partnerships, but also NGOs have taken an active role in exchanging the latest knowledge in specific fields, providing health services, and equipping the health sector with the most advanced medical devices. The fields of interventions have varied, from screening programs to diagnostics advances to detect infections and to prevent their spreading. The health needs of families with small children living in the most deprived settlements of the programme area were also tackled. When the war erupted, the health services were extended to Ukrainian internally displaced persons accommodated in the Western region, facing the same challenges as host communities regarding their needs. In some areas, the population increased by more than 40%, overloading the system. “Although at the time of planning we had a peaceful period – continues Nikoletta – one axe of cooperation among hospitals was already focusing on modern medical attendance of wartime injuries, the importance of which has become unfortunately more actual than ever in the last two years”.
Within the frame of the HSRU ENI CBC Programme, hospitals from the four countries have formed partnerships, but also NGOs have taken an active role in exchanging the latest knowledge in specific fields, providing health services, and equipping the health sector with the most advanced medical devices. The fields of interventions have varied, from screening programs to diagnostics advances to detect infections and to prevent their spreading. The health needs of families with small children living in the most deprived settlements of the programme area were also tackled. When the war erupted, the health services were extended to Ukrainian internally displaced persons accommodated in the Western region, facing the same challenges as host communities regarding their needs. In some areas, the population increased by more than 40%, overloading the system. “Although at the time of planning we had a peaceful period – continues Nikoletta – one axe of cooperation among hospitals was already focusing on modern medical attendance of wartime injuries, the importance of which has become unfortunately more actual than ever in the last two years”.
Curbing pathogens from border crossing

But let’s look at developments in the infectious diseases sector. “Cross-border partnership projects are exceptional opportunities for us”, says Attila Szűcs, director general of the Szabolcs-Szatmár-Bereg County Teaching Hospital (Hungary), lead partner in two initiatives, the “Infectious diseases have no borders” (IDHB) and “TBC has no borders” (TBCHB) implemented across Hungary and Ukraine. As we could see during the COVID era, pathogens can easily transit through administrative frontiers. “Cross-border migration is a massive phenomenon of our time – continues Mr Szűcs – Be it for war, subsistence, or tourism, within a few hours it can create the possibility for an infection to traverse several national borders and reach far from the place of origin. Thanks to our initiatives, we have reinforced the foundations of the health infrastructure and improved the diagnostic and treatment capacities of the partners, enabling the prevention of disease spreading”.
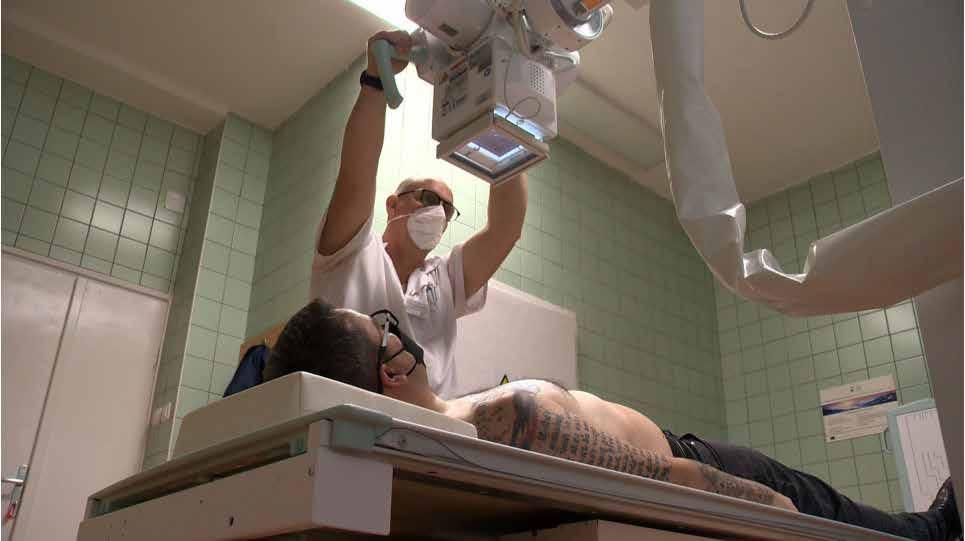
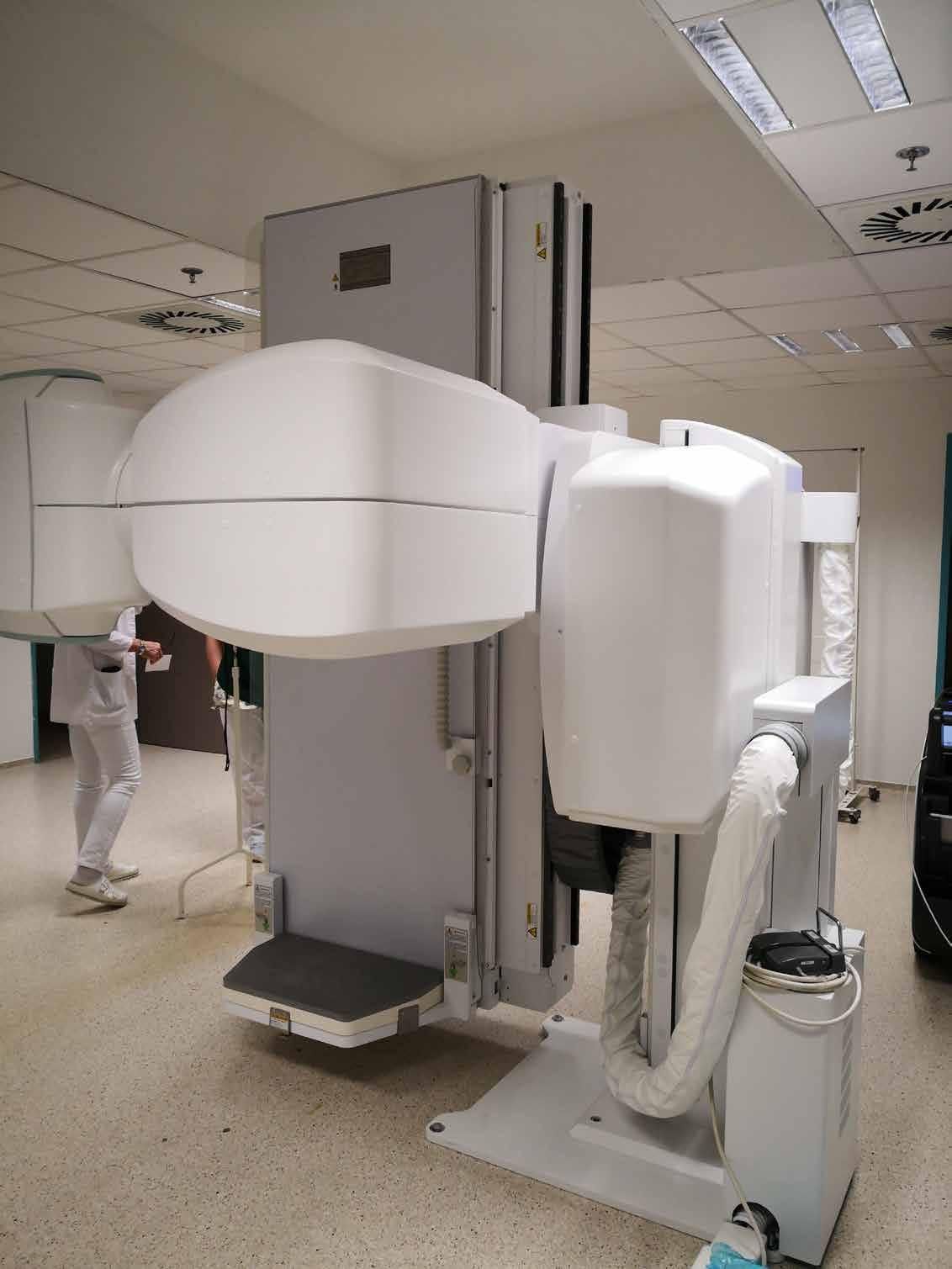 For both projects the approach was almost the same: to reduce the diffusion of infections associated with the increase of border traffic it was necessary to balance healthcare capacities between Hungary and Ukraine. This was done through professional guidance and training from the Hungarian side, in connection with the development of prevention, detection methods and early treatment of diseases. At the same time, there were works of modernisation of infrastructure in all three partner hospitals, including the acquisition of equipment.”We improved our outdated X-ray diagnostic park – continues the hospital director– with digital, low-radiation devices, which are much more efficient and can help in making more precise diagnosis, with lower radiation exposure”. At the Mukachevo Children’s Hospital – the Ukrainian partner – the infectious disease department was renovated, a bronchoscope device and other laboratory diagnostic equipment were also bought. In Uzhhorod Infectious Disease Hospital – a second partner from Ukraine – a new bacteriological laboratory was created. “Equipment development is very important – says Erzsébet Biró, director of the Subcarpathian County Children’s Hospital in Mukachevo, partner of both projects – but it is as important to be able to create a quality environment for healthcare workers and patients. Thanks to the project, we have completely renovated our department, as well as our water and sewage systems: both the patients and the staff are now placed in an environment of adequate quality”.
For both projects the approach was almost the same: to reduce the diffusion of infections associated with the increase of border traffic it was necessary to balance healthcare capacities between Hungary and Ukraine. This was done through professional guidance and training from the Hungarian side, in connection with the development of prevention, detection methods and early treatment of diseases. At the same time, there were works of modernisation of infrastructure in all three partner hospitals, including the acquisition of equipment.”We improved our outdated X-ray diagnostic park – continues the hospital director– with digital, low-radiation devices, which are much more efficient and can help in making more precise diagnosis, with lower radiation exposure”. At the Mukachevo Children’s Hospital – the Ukrainian partner – the infectious disease department was renovated, a bronchoscope device and other laboratory diagnostic equipment were also bought. In Uzhhorod Infectious Disease Hospital – a second partner from Ukraine – a new bacteriological laboratory was created. “Equipment development is very important – says Erzsébet Biró, director of the Subcarpathian County Children’s Hospital in Mukachevo, partner of both projects – but it is as important to be able to create a quality environment for healthcare workers and patients. Thanks to the project, we have completely renovated our department, as well as our water and sewage systems: both the patients and the staff are now placed in an environment of adequate quality”.
Preventing the spread of tuberculosis
Last but not least, the trainings. In the summer of 2021 the Ukrainian professionals of the Mukachevo and Uzhhorod hospitals had the opportunity to get acquainted with the methods and good practices used in Hungary not only in theory, but also in practice. ”We presented an infectious disease training, covering  infection-related control and methodologies -– continues Mr Szűcs – as well as a microbiological training, dealing with cultivation methods of bacteria, laboratory algorithms, rapid diagnostic and automation options“. Training was essential also for the TBCHB project, aimed at preventing the spread of tuberculosis. In order to suppress the disease caused by this bacterium – which primarily attacks the lungs, but also the kidneys, brain and lymphatic system – Hungarian doctors built a training series where pulmonologists from Mukachevo could learn about the diagnosis and treatment options for children, as well as about adults. Thanks to the sharing of know-how, the review of therapeutic options and the acquisition of appropriate equipment, project partners have reduced the existing disparities in the prevention and availability of early therapy for tuberculosis. It’s still too soon to measure the long-term impact, but the number of TBC cases should decrease on both sides of the border.
infection-related control and methodologies -– continues Mr Szűcs – as well as a microbiological training, dealing with cultivation methods of bacteria, laboratory algorithms, rapid diagnostic and automation options“. Training was essential also for the TBCHB project, aimed at preventing the spread of tuberculosis. In order to suppress the disease caused by this bacterium – which primarily attacks the lungs, but also the kidneys, brain and lymphatic system – Hungarian doctors built a training series where pulmonologists from Mukachevo could learn about the diagnosis and treatment options for children, as well as about adults. Thanks to the sharing of know-how, the review of therapeutic options and the acquisition of appropriate equipment, project partners have reduced the existing disparities in the prevention and availability of early therapy for tuberculosis. It’s still too soon to measure the long-term impact, but the number of TBC cases should decrease on both sides of the border.
From five days to few hours for virus identification
 The implementation of both projects has had a positive impact on the population of the region. Using the equipment purchased within the framework of the IDHB project, the time to identify disease-causing bacteria and viruses has been significantly shortened from five days to a few hours, so adequate therapy can start sooner, patients can receive targeted treatment more quickly, and the time of spreading is reduced. The upgrading of the hospitals’ infectious department is also shortening the hospitalization time. With the diagnostic tools acquired within the framework of the TBCHB, the time to establish the correct diagnosis has also been lowered, in addition to the fact that the higher quality image resolution enables more accurate diagnosis. But the reception was favourable not only from patients and healthcare workers: “The healthcare system as a whole is appreciative of our projects’ achievements – concludes Erzsébet Biró – I am thinking here about politicians and the county management: they see how the hospital can develop thanks to the European support and they feel encouraged to help us more”.
The implementation of both projects has had a positive impact on the population of the region. Using the equipment purchased within the framework of the IDHB project, the time to identify disease-causing bacteria and viruses has been significantly shortened from five days to a few hours, so adequate therapy can start sooner, patients can receive targeted treatment more quickly, and the time of spreading is reduced. The upgrading of the hospitals’ infectious department is also shortening the hospitalization time. With the diagnostic tools acquired within the framework of the TBCHB, the time to establish the correct diagnosis has also been lowered, in addition to the fact that the higher quality image resolution enables more accurate diagnosis. But the reception was favourable not only from patients and healthcare workers: “The healthcare system as a whole is appreciative of our projects’ achievements – concludes Erzsébet Biró – I am thinking here about politicians and the county management: they see how the hospital can develop thanks to the European support and they feel encouraged to help us more”.
Joining forces against tumor diseases
In 2020, 1.3 million people died of cancer in the EU, and the number of cases continues to rise. Lung cancer is the leading cause of death in men, and breast cancer in women. Tumors can be caused by a combination of genetic and environmental factors. Several types of cancer are related to causes such as the effects of smoking and alcoholism: but unfortunately, the chance of developing cancer increases with age, so prevention and maintaining a healthy lifestyle are essential. Without treatment, this uncontrolled cell proliferation leads to death, although today most forms of the disease can be cured, many of them completely if treatment is started in time. The chances of survival largely depend on how quickly and at what stage the disease is diagnosed. That is why four hospitals across four countries have decided to join forces to increase the efficiency of secondary prevention, particularly concerning women. By improving the conditions for breast screening, the 4DAGMEG4 project wanted to contribute to the reduction of early, avoidable deaths, to the increment of life expectancy, and to the decrease of inequalities accessing health care. The leading partner of the project is the St. Damján Greek Catholic Hospital (Hungary), whose director-general Henrik Dénes Hegyi has no doubts: “Thanks to the mammography and ultrasound machines procured with the project, we have performed so far 1,395 screenings; out of them, 62 women received a cancer diagnosis. But because of the early detection, they have gained years, and life. Their chances of survival is the main result of the project until now”. The radiology department was also rebuilt at the Királyhelmec Hospital (Slovakia), and equipment and infrastructures were consolidated with the sharing of know-how, the implementation of joint training and prevention programs, the development of human resources.
Next step is Interreg NEXT
The St. Damjan Greek Catholic Hospital is also involved in another cooperation activity for the care of high-risk patients requiring urgent and intensive care. The hospital is only 50 km (and a border) apart from its partner in Uzhgorod (Ukraine), and they are linked by a road which is troubled by high car traffic and road accidents. The two partners wanted to reduce the mortality of traumatic or intoxicated patients, as well as people under cardiology, cardiovascular or respiratory arrest. So they have developed an intensive care department in both hospitals, equipping it with new medical devices. Uniformed protocols have also been established, so that patients will be attended in the same manner, regardless of the side of the border they live on.
In conclusion, border regions face many challenges, a general shorter life expectancy, inequalities between and within countries. Their health systems withstand serious problems dealing with poverty and social exclusion, and the need for intervention is strong. Following its previous engagements – and considering the positive implications on society of a stronger and more inclusive health system – the Interreg NEXT Hungary-Slovakia-Romania-Ukraine Programme has decided to finance projects under health care with an increased amount, up to 20 million €.